The coronavirus that causes the coronavirus disease (COVID-19) has spread around the globe and is wreaking havoc. Earlier, this virus was found to affect the lungs and cause pneumonia, which resulted in breathing difficulties. As of now, the official list of COVID-19 symptoms is a dry cough, fever, chills, muscle pain, headache, sore throat, breathing difficulty, and loss of smell or taste (according to the Centers for Disease Control and Prevention). All these symptoms result from respiratory tract infections. But, recent studies have shown that this virus is capable of affecting almost every organ in the body, including the skin, brain, heart, and digestive tract.
Doctors across the globe have reported unusual symptoms in patients testing positive for the coronavirus (SARS-CoV-2). There have been reports of silent or “happy” hypoxia, where patients with dangerously low blood oxygen levels are not showing signs of breathing difficulties. Dermatologists have noted an increase in young patients with painful chilblains-like lesions in the toes, which they are calling “COVID toes.” Pediatricians reported symptoms similar to Kawasaki disease, such as inflammation of blood vessels throughout the body, in children. The other common complication that has been seen in COVID-19 patients is blood clots, which lead to strokes and pulmonary embolisms. Chickenpox-like rashes all over the body were also reported in some cases. It is interesting that a respiratory virus results in such a diverse array of symptoms and complications.
Respiratory symptoms are still the most common symptoms, but these atypical symptoms and complications should not be overlooked. Some patients might develop both typical and atypical symptoms, while others do not show any signs or symptoms (asymptomatic patients). This article is not to scare the readers, but is written with the aim of spreading awareness about the less common symptoms of COVID-19, which might help readers identify them.
The following are some atypical symptoms or complications associated with the new coronavirus infection:
COVID Toes
Amongst all the skin manifestations of COVID-19, a chilblains-like lesion on the feet of young adults and children is the most noteworthy. Chilblains are painful, and itchy, and appear as red papules, blisters, or swelling on the toes due to exposure to cold and humid climates. Similar lesions were first described in COVID-19 patients by dermatologists in China, and then in Italy, France, Spain, and Belgium.
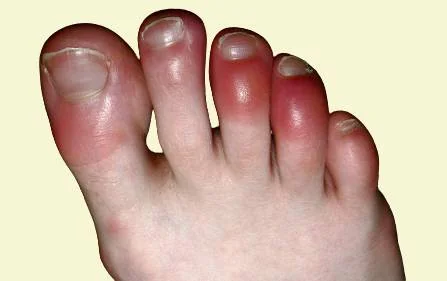
image-source : nytimes
As these lesions look similar to chilblains, they are called pseudo-chilblains, and as they are predominantly seen in toes, they are also known as COVID toes. COVID toes, unlike usual chilblains, appear in warmer climates, and tend to be more itchy, painful, and burning. They ulcerate more commonly and can take a longer time to heal.
Out of the 375 COVID-19 patients reported to have skin rashes in Spain, 19 % showed COVID toes. Most young patients with COVID toes remain otherwise asymptomatic. This symptom usually lasts for around 10 to 12 days and appears later in the course of the disease.
Other Skin Rashes
It is not new for viruses to cause skin rashes, as it is commonly seen in chickenpox, measles, herpes, etc. But what makes the coronavirus so unique is its potential to cause so many varieties of skin rashes. Apart from COVID toes, the following skin rashes have also been reported in those 375 patients-
-
Chickenpox-Like Lesions - In 9 percent of the cases, small itchy blisters were found in the limbs and trunk. These blisters lasted for about 10 days and were common in middle-aged patients.
-
Maculopapular Eruptions - In 47 percent of the patients, small and slightly raised red bumps were seen. These maculopapular lesions lasted for about seven days and were more common in patients with severe infections.
-
Urticaria - In 19 percent of the patients, hives-like pink or white, itchy, and raised lesions were reported. These were commonly appreciated in the palms.
-
Livedo or Necrosis - In older and critically ill patients, the skin turns red or blue due to poor blood circulation.
Even though these skin lesions were reported in many patients, they mostly occur along or after the respiratory symptoms, so they do not really help in diagnosing COVID-19.
Multisystem Inflammatory Syndrome in Kids
The CDC (Centers for Disease Control and Prevention), on May 14, reported a multisystem inflammatory syndrome in children (MIS-C) associated with the coronavirus. It has been reported in patients younger than 21 years and can result in unique symptoms.
This syndrome was first suspected in the United Kingdom on April 26, as an increasing number of children were getting admitted with a severe inflammatory syndrome. The symptoms resemble Kawasaki disease (a rare childhood disease that results in the inflammation of blood vessels throughout the body) and toxic shock syndrome (a fatal illness caused by toxins released by bacteria). The symptoms associated with this syndrome are:
-
Prolonged fever.
-
Stomach pain, vomiting, and diarrhea.
-
Reddish skin rashes.
-
Feet and hands swelling.
-
Enlarged lymph nodes.
-
Red and cracked lips.
-
Strawberry-like red tongue.
-
Swollen and red eyes.
Doctors believe this syndrome to be a result of children’s accelerated immune response to the virus, which leads to inflammation of the blood vessels and other symptoms.
Blood Clots and Strokes
Young coronavirus patients, those between 30 and 40 years of age, are experiencing a sudden loss of blood supply to some parts of the body due to unexplained blood clots of different sizes. Some of these blood clots block the blood supply to the brain, resulting in a stroke, or stopping the blood flow in the lungs, causing a pulmonary embolism (PE). Smaller blood clots block smaller arteries. The worst thing about these blood clots is that they do not respond to blood thinners and need surgery.
Blood clots have been associated with various viral infections, including SARS (severe acute respiratory syndrome). But there are reasons why scientists believe that a specific characteristic of this coronavirus is increasing the risk of blood clots in patients. Autopsy studies conducted on patients who died of COVID-19 showed blood clots in small vessels of the lungs, heart, liver and kidney.
Silent or “Happy” Hypoxia
This might be the most confusing COVID-19 symptom. The normal oxygen saturation in the blood is 95 to 100 percent. Hypoxia is when the oxygen levels in the body become low, which leads to symptoms like shortness of breath. More COVID-19 patients are presenting with a silent or “happy” hypoxia, meaning the patient can breathe normally when the body’s oxygen levels are below 90 percent. They do not develop shortness of breath, nor do their breathing becomes fast or shallow.
This can be dangerous because the patient is not aware of the dropping oxygen levels, and fails to get immediate help. The exact cause of silent hypoxia is not known.
Gastrointestinal (GI) Symptoms
The CDC included gastrointestinal symptoms like nausea, vomiting, and diarrhea to the list of COVID-19 symptoms. But, earlier studies suggest that these symptoms were not common in COVID-19 patients. According to a recent survey conducted on 116 COVID-19-positive patients, almost one-third had symptoms like nausea, loss of appetite, vomiting, or diarrhea.And these gastrointestinal symptoms can sometimes develop even before fever and other respiratory symptoms.
The stomach’s acidic environment kills the virus that enters the gut through the mouth (saliva). But, some scientists believe that people who take acidity medicines to neutralize stomach acids might be creating a perfect environment for SARS-CoV-2 to bind to ACE2 cell receptors present abundantly in the GI tract, which might lead to gastrointestinal symptoms. Researchers are trying to determine if these acidity drugs can increase the risk of a person developing GI symptoms.
Delirium and Other Neurological Symptoms
Researchers in the JAMA Neurology report delirium, confusion, disorientation, and other neurological symptoms to be associated with some people with COVID-19.
Some milder neurological symptoms like loss of taste, loss of smell, headache, muscle weakness, and dizziness can be seen early in patients, while the severe symptoms may develop later. Some patients have shown altered mental status and brain inflammation.
Eye Symptoms
Patients with severe infections have swollen eyelids, excessive watering, light-sensitive, itchy eyes and irritation. The blood vessels in the eyes look enlarged and red.
Loss of Smell or Taste
The CDC also included loss of smell or taste in the list of COVID symptoms. As these symptoms are seen in patients before they develop any other COVID-19 symptoms, it can be used as a screening criterion. According to a study published in the International Forum of Allergy and Rhinology, 68 percent of COVID-19 patients had impaired smell, 71 percent had impaired taste, and only 16 to 17 percent of patients had a loss of smell or taste. In a study it was found that changes in smell and taste often resolve within 30 days, but moderate to severe changes in smell and taste can last for 60 days or more.
Tinnitus
It is the feeling of something ringing in the ear. Research suggests that 19 percent or one in five of COVID- infected people have ear problems. The symptoms vary from person to person and they can range from high sequel to a low roar.
What Is the Reason Behind these Unusual Manifestations of COVID-19
Researchers have seen some of these symptoms, such as blood clots, in patients infected with the SARS and the H1N1 influenza virus also. They are working hard to find the exact mechanism behind this wide range of symptoms. For now, the immune system’s inflammatory response to the virus is said to result in blood clots.
Conclusion:
As this virus and its new variants are emerging, scientists and researchers find something new about SARS-CoV-2 every day. The symptoms listed in this article are based on various studies conducted on COVID patients all over the world. Having one or more of these symptoms does not mean that you are infected. The only sure way to know is by getting tested.
For more information, consult a doctor online now!
